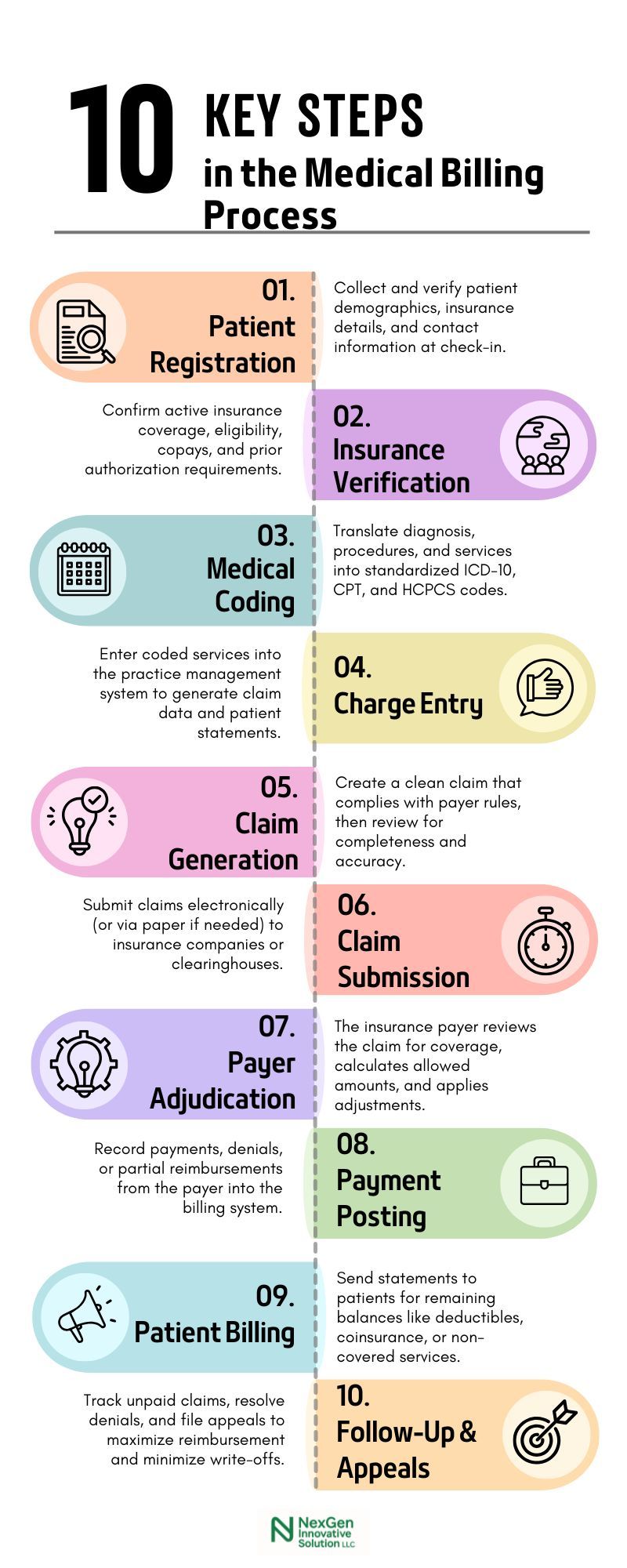
- Patient Registration
Collect demographic and insurance information accurately at intake. - Insurance Verification
Confirm coverage, eligibility, and prior authorization requirements. - Medical Coding
Translate diagnoses and services into standardized billing codes (ICD-10, CPT, HCPCS). - Charge Entry
Log coded services into the billing system for claim creation. - Claim Creation
Assemble a complete and clean claim, ready for submission. - Claim Submission
Transmit claims electronically to insurance payers or clearinghouses. - Payer Review & Adjudication
Insurer processes the claim, determines coverage, and issues payment decisions. - Payment Posting
Apply received payments, adjustments, or denials to the patient’s account. - Patient Billing
Generate and send statements for any patient-responsible balances. - A/R Follow-Up & Appeals
Track outstanding claims, address denials, and initiate appeals as needed.
💡 Accurate billing keeps your revenue cycle healthy, your compliance strong, and your patients informed.
Leave a Reply